Can games help improve infection prevention and control?
Hospital-acquired infections are serious business. Hundreds of millions of patients a year pick up infections significantly contributing to the global burden of disease. The problem is most acute in low- and middle-income countries where one in ten patients becomes infected contributing to untold suffering and placing significant strain on overstretched healthcare services.
The challenge of improving infection prevention and control (IPC) measures is multi-dimensional. There are significant structural constraints tied to the built environment. It is estimated that around a quarter of healthcare facilities lack basic water supply, which prevents people practising handwashing, whilst training and behavioural adherence issues among staff, patients and visitors also contribute to the infection burden.
Supported by the University of Leeds Crucible programme, we have begun a pilot project to assess the feasibility of using a game as a training aid for infection prevention and control. The idea is that the game helps users visualise infection risks within facilities and between patients and healthcare workers and that as part of a training module that can help users improve awareness of risk and strategies for minimising them. The underlying modelling framework of pathogen transmission has been developed with healthcare settings in the UK in mind, however, we will adjust the game experience to align especially for low resource healthcare settings.
The project involves colleagues from Civil Engineering and Mechanical Engineering at Leeds as well as the Women’s University in Africa, Zimbabwe, and Ark Foundation, Bangaldesh.
What’s in a game?
We all know games are instrumental in childhood learning and development, but it is also well established that games are great tools for supporting adult learning. They have even been games deployed previously in infection prevention and control training, although mainly deployed in high income contexts. In Figure 1 below we can see an early sketch of a possible interface for a game in which users could adjust parameters such as bed numbers, staff to patient ratios, hand hygiene practices and microorganism of interest, and assess the routes of transmission and implications for exposure and infection. The specific parameters will be matched to Zimbabwean and Bangladeshi health care operating contexts.
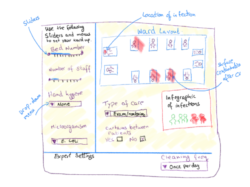
Figure 1 - Sketch of infection prevention and control game interface
We believe this sort of interface could be usefully deployed on phones, tablets or computers as part of a broader learning module on IPC. We are approaching the design of the game and learning module from a user-centred design approach so will be working with healthcare practitioners in Bangladesh and Zimbabwe to develop a design brief to work towards. One of the things that really excites me about the project is the use of the game to fairly demonstrate the possibilities for IPC within resource constrained healthcare facilities.
In a recent paper paper on Water, Sanitation and Hygiene practice within household settings, myself and co-authors discuss the ethical problems with expecting people living with limited infrastructure to maintain levels of hygiene necessary to protect them from faecal-oral disease transmission. Without accessible water supply, appropriate sanitation, and a living environment conducive to cleaning, it is very hard to wash hands, bodies and homes enough to reduce exposures to excreta related pathogens. Moreover, to expect people to do this is unfair and unethical.
This is a useful analogy when thinking about IPC in resource constrained healthcare settings. When working with very low staff-to-patient ratios, limited handwashing facilities, and unregulated access of visitors into clinical areas, it is extremely difficult to practice effective IPC. I am hopeful we can create a game and learning experience that is sympathetic to this reality and which can be useful as a training aid. But, more broadly, promote wider learning and advocacy about improving healthcare facilities and services to a level in which IPC can be effectively practiced.
Assessing feasibility and next steps
An important thing to articulate about this project is that it is a pilot project and only setting out to test the feasibility of this sort of approach, rather than a formal evaluation of its effectiveness from a clinical or any other perspective. When assessing feasibility, we are interested in what healthcare workers in Bangaldesh and Zimbabwe really think about this approach and how it would fit into existing training and support initiatives.
More broadly, I am conscious that we are also assessing the feasibility of ourselves as a group of researchers to lead such an initiative. We are hoping to engage with people already working in this area or with the approaches we are using – such as the serious game approach – to learn from them.
Looking forward, we hope the process provides enough learning and encouragement for us and other collaborators to build on the work to upscale from feasibility to a more formal design and evaluation process. As such, we’d love to hear from anyone interested in this space or to hear your feedback on these ideas. Feel free to contact me - Dr Paul Hutchings at: p.hutchings@leeds.ac.uk.
